In California, the passage of SB 863 signaled yet another attempt to control the costs of the $16 billion a year workers compensation system, by reducing costs and promoting efficiency, but also increasing the benefits to injured workers for permanent disability. In review of SB 863, there are many positive aspects that will help in the reduction of permanent disability, but there are also elements to the reform that may have negative consequences on your claim costs.
First, the positive: SB 863 eliminates the allowance for permanent disability due to “add-ons” such as psych, sexual dysfunction and sleep disorders. These were costly additions that in our experience were rarely supported by objective evidence. In litigated cases, the disallowance of these add-ons will generate significant cost savings.
Now, the negative: While the FEC adjustment has been eliminated, making the rating strand a little less complicated, all whole person impairment ratings are now automatically provided an adjustment factor of 1.4. This was the highest FEC modifier under the old schedule, and means that all cases will see an increase in permanent disability percentages. On top of this, the legislature added hundreds of billions of dollars to the permanent disability schedule, and will phase in a max rate of $290 per week by 2014.
Our overall analysis is that while the problems of add-ons have been eliminated, these did not impact all cases. What will impact all cases is the max FEC adjustment, and the increase in value in the PD schedule. Our data, consistent with that published by the AMA in 2010, shows that there is a significant error rate in whole person impairment ratings assigned in California, about 70%, and that the rating assigned is typically twice what it should be. When factoring in the allowance for Almaraz/Guzman, SB 863 will provide little relief for the erroneous ratings being assigned in California, and has only exacerbated the costs of these errors.
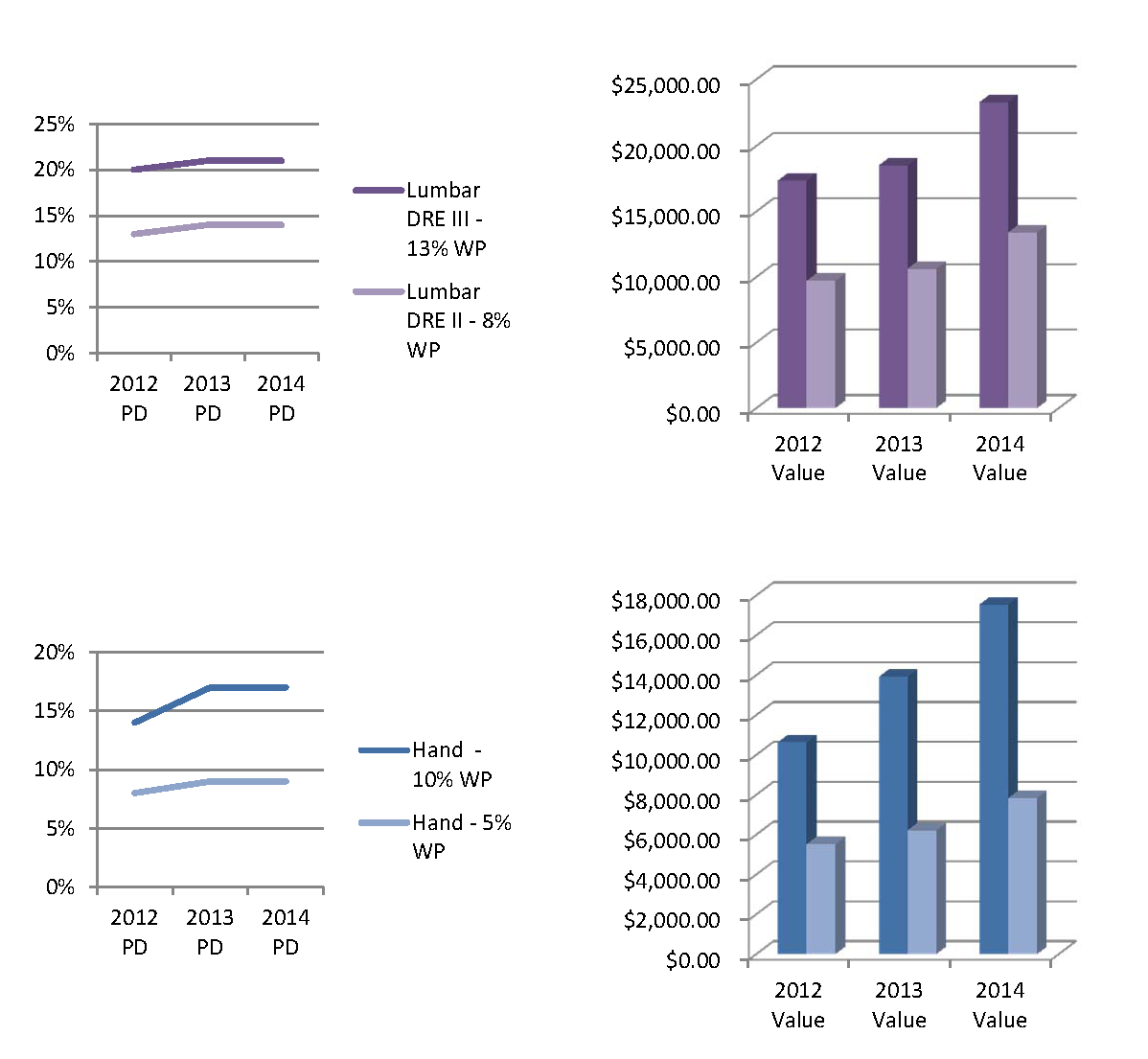
For example, we took two common types of errors that we find in our reviews. The first is a lumbar spine injury that was assigned a DRE Lumbar Category III rating of 13% WP when the findings in the case would only support a DRE Lumbar Category II rating of 8% WP. The second is a multiple digit/hand injury that was assigned 10% whole person when the findings actually support a rating of 5% whole person. The charts below show the difference in value included in SB 863, and what the legislative changes mean when there is an error in the rating (examples use age at DOI of 45 and occ code of 350).
As illustrated above, an overrating of only 5% WP in the lumbar spine rating would currently result in a potential PD over payment of $7,648. After the reform, this error will cost $9,933. For the hand injury, an overrating of 5% WP would currently result in an over payment of $5,118. After the reform, this error will cost nearly twice that, at $9,715.
Therefore, once SB 863 takes full effect, it will be more important than ever to ensure that permanent disability on your files is based on an accurate impairment rating. Based on the historical evidence of error rates in California, the survival of Almaraz/Guzman, and the increase in both PD percentages and values allowed in SB 863, the cost of these errors will only increase, and could potentially offset any cost reductions brought about in the reform.